Welcome to DU!
The truly grassroots left-of-center political community where regular people, not algorithms, drive the discussions and set the standards.
Join the community:
Create a free account
Support DU (and get rid of ads!):
Become a Star Member
Latest Breaking News
Editorials & Other Articles
General Discussion
The DU Lounge
All Forums
Issue Forums
Culture Forums
Alliance Forums
Region Forums
Support Forums
Help & Search
General Discussion
Related: Editorials & Other Articles, Issue Forums, Alliance Forums, Region ForumsMore people than ever are hospitalized with COVID-19. Health-care workers can't go on like this.

https://www.theatlantic.com/health/archive/2020/11/third-surge-breaking-healthcare-workers/617091/
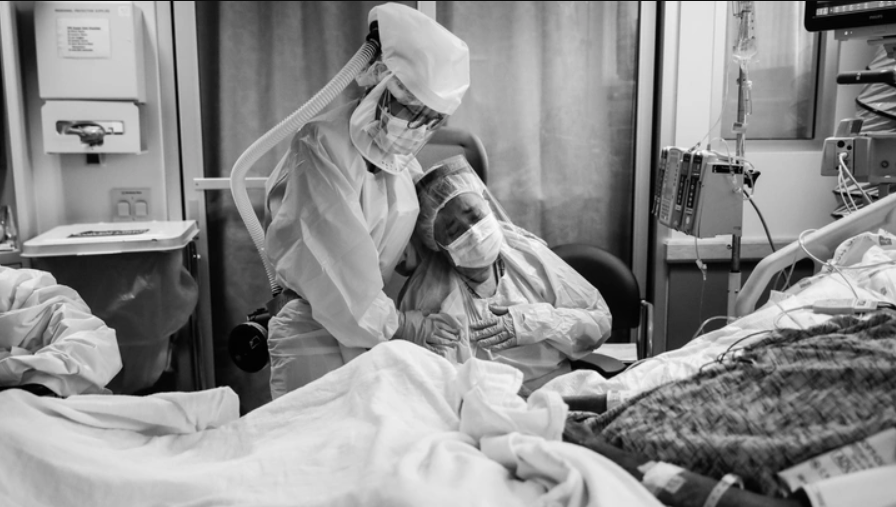
On Saturday morning, Megan Ranney was about to put on her scrubs when she heard that Joe Biden had won the presidential election. That day, she treated people with COVID-19 while street parties erupted around the country. She was still in the ER in the late evening when Biden and Vice President–elect Kamala Harris made their victory speeches. These days, her shifts at Rhode Island Hospital are long, and they “are not going to change in the next 73 days,” before Biden becomes president, she told me on Monday. Every time Ranney returns to the hospital, there are more COVID-19 patients. In the months since March, many Americans have habituated to the horrors of the pandemic. They process the election’s ramifications. They plan for the holidays. But health-care workers do not have the luxury of looking away: They’re facing a third pandemic surge that is bigger and broader than the previous two. In the U.S., states now report more people in the hospital with COVID-19 than at any other point this year—and 40 percent more than just two weeks ago.
Emergency rooms are starting to fill again with COVID-19 patients. Utah, where Nathan Hatton is a pulmonary specialist at the University of Utah Hospital, is currently reporting 2,500 confirmed cases a day, roughly four times its summer peak. Hatton says that his intensive-care unit is housing twice as many patients as it normally does. His shifts usually last 12 to 24 hours, but can stretch to 36. “There are times I’ll come in in the morning, see patients, work that night, work all the next day, and then go home,” he told me. I asked him how many such shifts he has had to do. “Too many,” he said. Hospitals have put their pandemic plans into action, adding more beds and creating makeshift COVID-19 wards. But in the hardest-hit areas, there are simply not enough doctors, nurses, and other specialists to staff those beds. Some health-care workers told me that COVID-19 patients are the sickest people they’ve ever cared for: They require twice as much attention as a typical intensive-care-unit patient, for three times the normal length of stay. “It was doable over the summer, but now it’s just too much,” says Whitney Neville, a nurse based in Iowa. “Last Monday we had 25 patients waiting in the emergency department. They had been admitted but there was no one to take care of them.” I asked her how much slack the system has left. “There is none,” she said.

The entire state of Iowa is now out of staffed beds, Eli Perencevich, an infectious-disease doctor at the University of Iowa, told me. Worse is coming. Iowa is accumulating more than 3,600 confirmed cases every day; relative to its population, that’s more than twice the rate Arizona experienced during its summer peak, “when their system was near collapse,” Perencevich said. With only lax policies in place, those cases will continue to rise. Hospitalizations lag behind cases by about two weeks; by Thanksgiving, today’s soaring cases will be overwhelming hospitals that already cannot cope. “The wave hasn’t even crashed down on us yet,” Perencevich said. “It keeps rising and rising, and we’re all running on fear. The health-care system in Iowa is going to collapse, no question.” In the imminent future, patients will start to die because there simply aren’t enough people to care for them. Doctors and nurses will burn out. The most precious resource the U.S. health-care system has in the struggle against COVID-19 isn’t some miracle drug. It’s the expertise of its health-care workers—and they are exhausted.
The struggles of the first two COVID-19 surges in the United States helped hospitals steel themselves for the third. Hardened by the crucible of March and April, New York City built up its ability to spot burgeoning hot spots, trace contacts, and offer places where infected people can isolate. “We’re seeing red flags but we’ve prepared ourselves,” says Syra Madad from NYC Health + Hospitals. Experienced health-care workers are less fearful than they were earlier this year. “We’ve been through this before and we know what we have to do,” says Uché Blackstock, an emergency physician who works in Brooklyn. And with the new generation of rapid tests, Blackstock says she can now tell patients if they have the coronavirus within minutes—a huge improvement over the spring, when tests were scarce and slow. Smaller clinics, nursing homes, and long-term-care facilities are still struggling to provide personal protective equipment, including gloves and masks. “About a third are completely out of at least one type of PPE” despite having COVID-19 cases, says Esther Choo, a physician at Oregon Health and Science University and a founder of Get Us PPE. But larger hospitals are doing better, having built up stockpiles and backup plans in case supply chains become strained again. “The hospital is probably the safest place to work in Iowa, because we actually have PPE,” Perencevich said.
snip
4 replies
 = new reply since forum marked as read
Highlight:
NoneDon't highlight anything
5 newestHighlight 5 most recent replies
= new reply since forum marked as read
Highlight:
NoneDon't highlight anything
5 newestHighlight 5 most recent replies
More people than ever are hospitalized with COVID-19. Health-care workers can't go on like this. (Original Post)
Celerity
Nov 2020
OP
JCMach1
(29,143 posts)1. The Winter Wave is just getting started, unfortunately
elias7
(4,229 posts)2. As a health care worker, this is square at the feet of administration, Covid deniers
Roisin Ni Fiachra
(2,574 posts)3. And Trump supporters just don't care. nt
hunter
(40,476 posts)4. It's horrible. My wife is a health care professional.
This article describes what she is experiencing.
Making matters worse, patients with other medical problems are sicker than usual, several doctors told me. During the earlier surges, hospitals canceled elective surgeries and pulled in doctors from outpatient clinics. People with heart problems, cancers, strokes, and other diseases found it harder to get medical help, and some sat on their illness for fear of contracting COVID-19 at the hospital. Now health-care workers are facing an influx of unusually sick people at a time when COVID-19 has consumed their attention and their facilities. “We’re still catching up on all of that,” says Choo, the Oregon physician. “Even the simplest patients aren’t simple.”
